Welcome To Our Blog

Numbness and Tingling in an Arm or Leg
Numbness or tingling in an arm or leg is a sign to seek help and evaluation from a spine specialist. Referred to as radiculopathy, this numbness or tingling in the extremities is caused when one or more spinal nerve roots are compressed, irritated, or inflamed.

Pinched Nerve – A Common Cause of Back and Neck Pain
Pinched nerves are a common cause of neck or back pain. Nerves can become compressed, irritated, or inflamed and this leads to a variety of uncomfortable and sometimes debilitating symptoms. Pinched nerves can happen when there is a herniated disc, bone spurs, spinal stenosis, muscle tightness, or repetitive motion injuries.

The Best Advice – Act with Kindness
Dr. Victoria Knoll was recently interviewed by the American Society for Surgery of the Hand (ASSH) for their November newsletter. She had one piece of advice as we enter this holiday season - Act with Kindness. “What is a piece of advice you have received that has stuck with you? How do you apply it professionally and/or personally?” At first, I thought, this is hard. I have received a lot of good advice over the years. Then I thought more, and realized, this is actually quite easy. The best advice I have received was as a young child. Act with kindness: act with the...

Dr. James Guess Retires After 30 Years of Service.
After 30 years of practicing medicine, Dr. James Guess will be retiring on December 22, 2023. Dr. Guess began his career in orthopedics in 1995 with Southwest Orthopedics. In 1997, the name changed to Metrocrest Orthopedics and Sports Medicine. He practiced there until 2011 when the group merged with 3 other orthopedic groups and formed OrthoTexas. He has been the Medical Director of Baylor Scott & White Surgicare of Carrollton for 21 years. He has been the Chairman of Spine Surgery at Baylor Scott & White Medical Center of Frisco for the past 4 years and the Chairman...
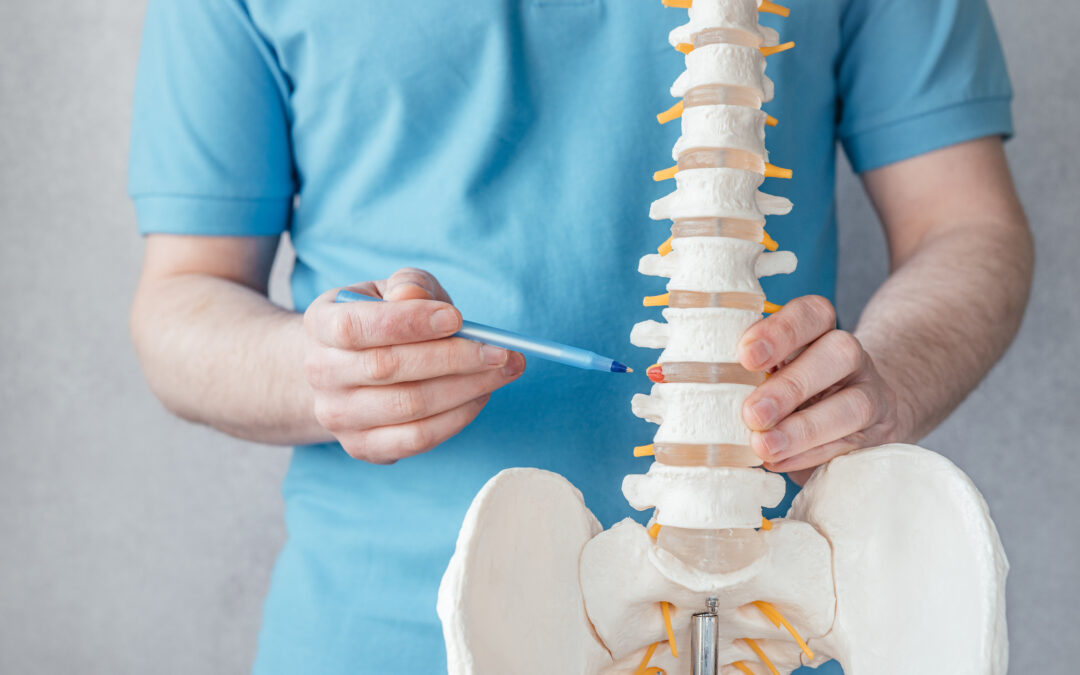
Disc Replacements Can Relieve Back Pain
Neck and back pain are a problem for more than 16 million Americans. It often results in chronic pain that can limit even everyday activities. In the past, the only surgical option was a fusion where the problem disc was removed, and the bones were fused together. Today, we have artificial discs that can replace the injured disc and can preserve motion in the neck or the back.
