Welcome To Our Blog

Fix the Part That Hurts: Partial Knee Replacement
When knee pain makes everyday movement feel like a battle, it’s easy to assume that a full knee replacement is the only solution. But for many patients, the damage is isolated to just one part of the joint. That’s where partial knee replacement offers a smarter, less invasive path to relief. Dr. Brian Fuller, an orthopedic surgeon at OrthoTexas, performs partial knee replacements to help patients get back on their feet faster with a gentler surgical impact and a more natural feel. This targeted procedure addresses only the damaged area, preserving healthy bone and tissue...

Total Ankle Replacement: What You Need to Know
Total ankle replacement is a surgical procedure designed to relieve pain and restore mobility in individuals suffering from severe ankle arthritis. Similar to a total knee replacement, this procedure involves removing the damaged joint and replacing it with a metal component on both the talus and tibia sides, with a plastic spacer in between that allows for smooth movement. Ankle Replacement vs. Ankle Fusion One of the most significant differences between ankle replacement and ankle fusion is mobility. Ankle fusion eliminates movement in the joint by using plates and screws to...
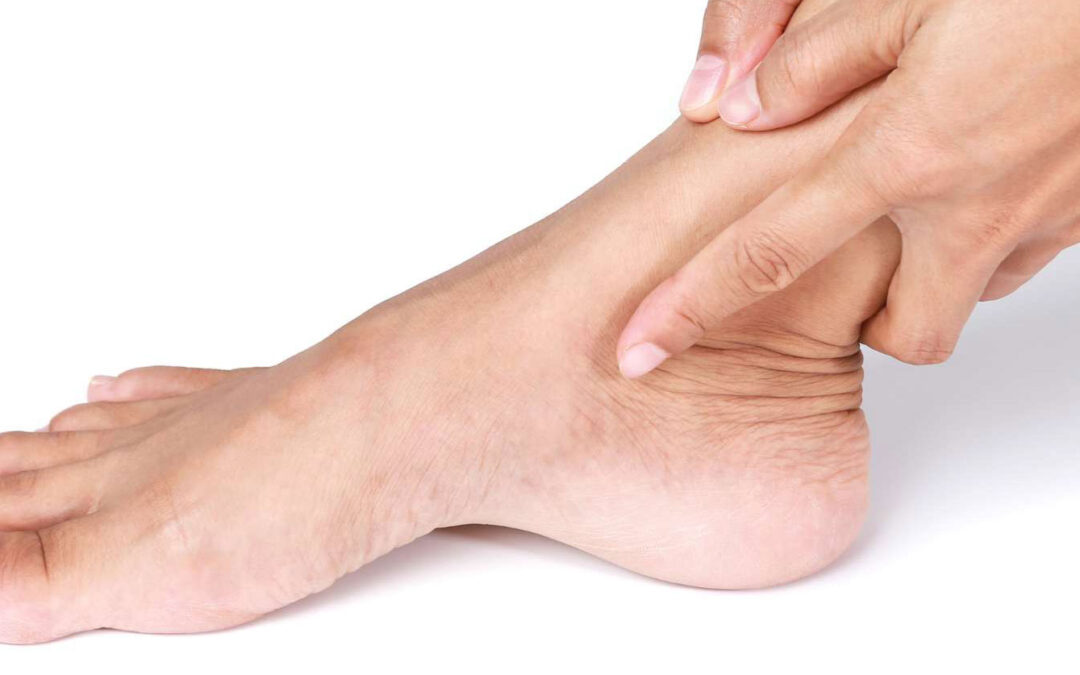
Ankle Ligament Reconstruction: What You Need to Know
Ankle injuries are common, but when they become chronic and impact daily activities or athletic performance, ankle ligament reconstruction may be necessary. This procedure helps restore stability, reduces the risk of future injuries, and allows individuals to regain confidence in their movement.Understanding Ankle Ligaments The ankle is supported by several key ligaments that play a crucial role in maintaining balance and preventing excessive movement. The deltoid ligament, located on the medial (big toe) side of the ankle, prevents the foot from turning too far outward. On...

Notice For Dr. Jason Alder’s Patients
Notice for Dr. Jason Alder's Patients Dr. Jason Alder will be leaving OrthoTexas on November 29, 2024. Our spine specialists, Shikha Sethi, MD and Aine McKenzie, MD are accomplished and experienced physicians that are more than happy to take over your care at our practice. In addition, we have two spine surgeons from Texas Spine Consultants that will be officing onsite at our Frisco and Carrollton locations to assist with the transition of your care. Chester Donnally, MD will be available in our Carrollton location, and A.J.Rush III, MD will be in our Frisco location. You can...

Thumb Arthritis – A Common Problem
Thumb arthritis, or basal joint arthritis, is a form of osteoarthritis that occurs in the thumb joint. It occurs at the base of the thumb, where the thumb meets the wrist. It is common, especially in people over the age of 50. In fact, 25% to 33% of people over 50 are estimated to have some degree of thumb arthritis. It is also more common in women, especially post-menopausal women, than in men. Some studies suggest that women are two to six times more likely to develop this condition than men. While not everyone with thumb arthritis experiences significant symptoms, it can...

